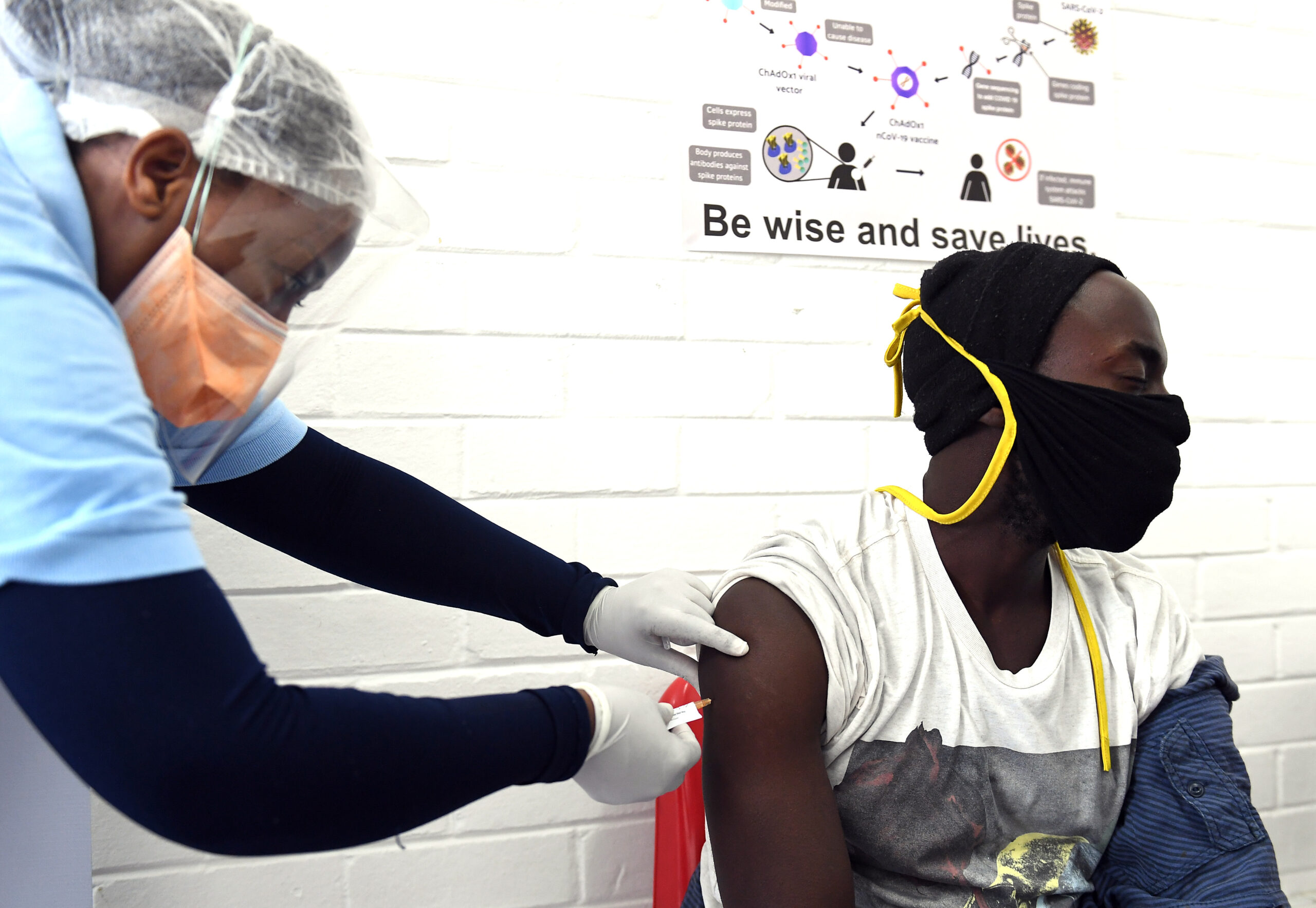
Mass vaccination remains one of the most successful, cost-effective public health interventions. Being vaccinated means individuals are not only protected from being infected themselves, they also cannot pass the infection onto other people, where it may cause severe disease.
However, stopping the continued spread of pathogens in a population requires herd immunity, also known as population immunity. Herd immunity is the indirect protection from an infectious disease that happens when a population is immune, either through vaccination or immunity developed through previous infection.
Experts have warned that around 80-90% of specific populations must have Covid-19 immunity, either through prior infection or vaccination, to reach herd immunity, but seroprevalence studies suggest that less than 10 percent of people in most countries have been infected with Covid-19. The World Health Organisation (WHO) supports achieving herd immunity through vaccination, not by allowing a disease to spread through any segment of the population, as this would result in unnecessary cases and deaths.
Therefore, safe and effective mass vaccination is by far the preferable path to eradicating Covid-19.
The risks of vaccine nationalism
Glaring cases of vaccine nationalism have dampened the enthusiasm that greeted the record-breaking development of a Covid-19 vaccine. According to social justice campaign group Global Justice Now, 82% of the 1.35-billion Pfizer-BioNTech Covid-19 vaccine doses that will be produced by the end of 2021 have already been bought by the richest governments, representing only 14 percent of the global population. The same goes for Moderna’s Covid-19 vaccine. Of the 1-billion doses Moderna says it has the capacity to produce by the end of 2021, 780-million doses have been already been sold to rich governments. The every-country-for-itself approach has led to concerns that nearly a quarter of the world’s population may not have access to Covid-19 vaccines until at least 2022. The unequal allocation of vaccines could cost the global economy up to $1.2-trillion a year in GDP terms.
Covid-19 vaccination qualifies as public good. The pandemic can only be eradicated through vaccination of sufficient global population coverage. It is, therefore, important for vaccination to be available to everyone, everywhere. However, it is important to note that access to the future vaccine should be available to all – fairly and affordably – and not free, as acknowledged at the 73rd World Health Assembly, on 19 May 2020. The Assembly voted for a resolution calling for “universal, timely and equitable access to, and fair distribution of, all quality, safe, efficacious and affordable essential health technologies and products […], that are required in the response to the Covid-19 pandemic as a global priority, and the urgent removal of unjustified obstacles thereto.”
The Covid-19 vaccine global access facility (Covax), a vehicle of multilateral cooperation led by the WHO, the Coalition for Epidemic Preparedness Innovations, and Gavi plan to buy Covid-19 vaccines in bulk and distribute two-billion doses equitably around the world. This approach should provide enough doses for 20 percent of the people in the developing world by the end of 2021.
This represents a small fraction of the vaccines to be produced and is a far cry from the number required, even with the additional 270-million vaccines obtained by the African Union, to achieve herd immunity in Africa, home of the majority of least developed countries.
The total cost of vaccinating Africa’s population against Covid-19 is difficult to gauge, but the cost of vaccinating the priority populations in Africa is expected to be around $7-billion. This is far beyond the pressurised public purse of African countries.
Close to 900-million doses have been secured through multiple initiatives that include the Covax facility and the African Export-Import Bank-facilitated vaccine acquisition (Afreximbank). Afreximbank will, through its pandemic trade impact mitigation facility, provide advance procurement commitment guarantees of up to $2-billion to the manufacturers on behalf of member states. However, the question remains: how will least-developed African countries meet the current financial requirement and those of future vaccinations against possible epidemics? One innovative finance mechanism is vaccine bonds.
The case for vaccine bonds
The International Finance Facility for Immunisation (IFFIm) is one of the vital components of Gavi’s capital structure. IFFIm was founded in 2006 on the idea that private investors and government donors can work together to have a greater, more immediate impact on global health. Vaccine bonds have raised more than $6.4-billion from investors, making large volumes of funds immediately available for Gavi programmes. IFFIm funding has helped Gavi immunise more than 822-million children, averting 14 million deaths. “IFFIm’s vaccine bonds prove that investments can make both financial sense and a social impact by saving lives,” said IFFIm chair René Karsenti.
As with conventional and labelled bonds, vaccine bond issues represent borrowed funds over a period, and investors or creditors receive a coupon with a fixed or variable rate of return. The main difference between them is the use of the proceeds. Vaccine bonds mobilise tens of billions of dollars to vaccinate the developing world. According to Karsenti, “Vaccine bonds are critical testimony of the formidable evolution of the international bond markets, providing effective financing tools for social impact.”
IFFIm issued a 2-billion Norwegian krona bond, whose proceeds would contribute to the development of a Covid-19 vaccine. Crédit Agricole CIB acted as a joint bookrunner for the first Covid-19 Vaccine Bond issued by the IFFIm.
Central American Bank for Economic Integration (CABEI) is the first multilateral development bank to issue a Covid-19 vaccine bond with directed best efforts towards the acquisition of vaccines for the Central American population. The $50-million bond issuance is part of CABEI’s Covid-19 emergency programme.
Further progress has been made as the social bond market mobilises to combat Covid-19, although not specifically to pay for vaccines. The International Finance Corporation, the African Development Bank (AfDB), Council of Europe Development, the European Investment Bank, the Inter-American Development Bank, the Nordic Investment Bank, the Italian Development Bank and Swedish medical supplier Getinge are some notable issuers of labelled Covid-19 bonds.
Labelled Covid-19 bonds are not restricted to supranational organisations, multilateral development banks and investment banks. Any type of issuer, first-time or seasoned, can issue a labelled Covid-19 bond, provided their evaluation is based on four core components: use of proceeds, project selection process, management of proceeds and reporting, as outlined in the social bond principles and the sustainability bond guidelines supported by the International Capital Market Association.
There is a unique opportunity in Africa to build on the experiences of past issuances of labelled bonds by the AfDB, federal government of Nigeria, South African government, Industrial Development Corporation of South Africa, BMCE Bank of Morocco, Casablanca Finance City, Groupe Al Omrane and Access Bank Plc to raise the finance required to combat the pandemic on the continent. The success of these issuances shows the future looks positive for vaccine bonds in Africa.
The impact of Covid-19 on lives and livelihoods in Africa is stark. Socially conscious bond investors can meet funding challenges for Covid-19 while building knowledge, experience and competencies for possible future issuance. Furthermore, for African countries and governments, a tax-free labelled bond has significant potential to do the heavy lifting in the fight against Covid-19.